Normal bladder function
The bladder stores urine and acts like a balloon and fills up gradually and should hold around a pint (500ml) of urine. The kidneys produce urine and the amount depends on the volume of fluid consumed and activity.
It is normal to pass urine up to 6-8 times during the day and once at night. The amount of fluid you drink will effect how often you need to pass urine. For most people the average fluid intake should be approximately 1.5 – 2 litres a day.
Normal bladder muscle called detrusor muscle remains relaxed when filling up and the small muscles at the outlet of the bladder (urethra) remain contracted with extra support from the pelvic floor muscles to maintain continence and avoid leakage of urine.
Normally one goes to pass urine when it is socially appropriate and at this time, the bladder muscles contracts and the small muscles at the outlet (urethra) and pelvic floor muscles relax and the bladder is emptied. This mechanism is maintained by complex messages between the brain, bladder and pelvic floor muscles.
To remain continent (dry) the small muscles at the outlet (urethra) and bladder neck (where the urethra joins the bladder) must tighten under ‘stress- related’ conditions (e.g. when you cough, sneeze or exercise). Any disruption to this mechanism or weakness of the pelvic floor muscles may result in problems urinary leakage- stress incontinence.
Stress incontinence is the complaint of urinary leakage during any activity that increases pressure within the abdomen (tummy), such as coughing, sneezing or exercise.
It is a very common problem that affects about in 3 women at some point.
What causes stress incontinence?
Stress incontinence results from weakened or damaged pelvic floor muscles and inadequate support of the small muscles around the bladder outlet (urethra) and the junction to the bladder (bladder neck).
Weakening of the pelvic floor muscles is quite common after childbirth.
Chronic constipation, menopause (due to the loss of hormones), heavy or repeated lifting, persistent cough and excess weight gain are other causes of stress incontinence.
How is it diagnosed?
The diagnosis can be made from your complaints and by completing a bladder diary. Tests to assess the bladder function (urodynamics) may be required.
Lifestyle interventions
Weight loss, constipation avoidance and smoking cessation are simple helpful lifestyle interventions that are helpful.
Pelvic floor exercise
Pelvic floor exercise is the first step in managing mild symptoms and has up to a 70% chance of cure if performed correctly and consistently. You will need the expertise of a women’s health physiotherapist for pelvic floor assessment and muscle training.
Surgery
If symptoms remain bothersome despite pelvic floor training then surgery is an option. There are two main surgical interventions to treat stress incontinence.
Tension free Vaginal Tape Obturator- (TVT-O)
This procedure is performed under anaesthetic and involves the placement of a piece of non- dissolving tape (prolene mesh) through a small cut on the front wall of the vagina and out through a cut in the groin area. This has an excellent cure rate in excess of 90% but is served for women who have completed childbearing.

TVT-O
Urethral Bulking Agents
This involves the injection of particles into the wall of the small muscles at the bladder outlet (urethra) to support the closing mechanism.
Urethral bulking agent
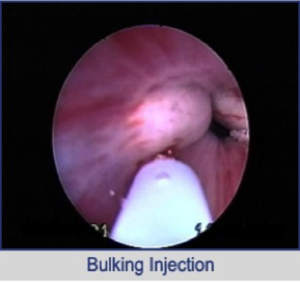
This is ideal for childbearing women and those with multiple medical problems who wish to avoid invasive surgery. The cure rate is 65% but it is less effective with time and repeat injections may be necessary.
Further details on the procedure to treat your symptoms will be discussed at your consultation.
For more information visit www.bladderandbowelfoundation.org/